When you discover that you’re pregnant …
 … you may begin to imagine the future and ultimate delivery of your baby. You imagine your belly growing as your baby grows to full term and you prepare to deliver as your due date approaches. You imagine that Immediately after your child is born, your healthy newborn is gently placed in your happy, exhausted arms. You spend some precious time holding or putting your baby to your breast, and you bask in one of the most rewarding and wonderful moments of your life. You then see yourself surrounded by flowers and balloons, proudly holding (and showing off) your baby as you leave the hospital or birthing center ready to embark on your new life as a mommy!
… you may begin to imagine the future and ultimate delivery of your baby. You imagine your belly growing as your baby grows to full term and you prepare to deliver as your due date approaches. You imagine that Immediately after your child is born, your healthy newborn is gently placed in your happy, exhausted arms. You spend some precious time holding or putting your baby to your breast, and you bask in one of the most rewarding and wonderful moments of your life. You then see yourself surrounded by flowers and balloons, proudly holding (and showing off) your baby as you leave the hospital or birthing center ready to embark on your new life as a mommy!
Things, however, don’t always turn out as we imagined they would.
When your baby arrives prematurely, it is usually a sudden, unexpected event which leaves your head spinning in shock and disbelief. Aside from the situations where a baby is intentionally delivered early due to a life-threatening condition involving the mother, child or both, many premature deliveries occur simply because of membrane rupture (water breaking) with or without prior warning. This is especially true with a multiple pregnancy.
Because the uterus is carrying more than one baby, it is not only growing larger than it would with a single pregnancy, but because of the faster rate of growth, it can become what is referred to as “irritable”. Yes, your uterus can develop a really bad attitude. With normal growth, the uterus stretches and contracts throughout pregnancy, but increased irritability causes contractions that are more than simple stretches. Contractions can become productive, which means that they cause cervical changes such as premature effacement (shortening) and dilation (opening), which begins the process of labor. In the case of premature labor, your doctor may place you on anti-contraction medication which often stops the labor process. In serious situations where labor is difficult to stop, or that has the potential for starting again, you will be placed on partial or complete bed rest until you reach a safe gestation (approximately 34 weeks and beyond) for the baby(ies) to be born.
When Premature Labor Cannot Be Stopped
Despite all of the efforts to postpone the delivery of your babies, quite often, they come anyway.
Following the whirlwind of your early delivery, either via vaginal or C-Section, suddenly there you are: no longer pregnant.
You may be feeling a combination of: shock, trauma, anger, disappointment, loss, fear and a shameful sense of self-failure. I know this, because I experienced all of those feelings after the birth of my first set of twins at 30 weeks and five days. After months on bed rest and anti-contraction medication, no further efforts were able stop my contractions, and my baby girls were born at 2 lbs., 14 oz. and 3 lbs., 1 oz.
Immediately after each baby was born, she was whisked away to the Neonatal (newborn) Intensive Care Unit (NICU). There were no sweet, warm bundles placed in my arms.
Adjusting to Reality
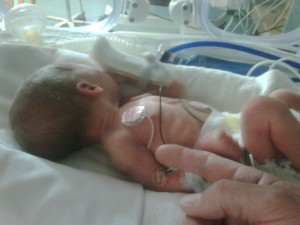 Unlike the way you always imagined, your babies are now completely under the care of the hospital neonatologist (newborn specialist physician) and of the NICU nurses. You’ve now entered a strange new world, as I did three times. As I mentioned, my first set of twins were born at 30 weeks and 5 days, and stayed hospitalized for 6 weeks. My second set were born at 35 weeks, 2 days, and although my son and daughter were born more than a month later than my first set, they were still considered premature (at 4 lbs., 13 oz. and 4 lbs., 6 oz.) and were again, taken away immediately after birth to the NICU, where they stayed just over a week. My third set threatened to come early as well, and although I was the model patient who did exactly as prescribed by my doctor (and myself), my baby boys were born (believe it or not) at 30 weeks and 5 days … exactly the same gestation as my first set, but their birth weights were heavier at 3 lbs., 11 oz. and 4 lbs., 1 oz. They stayed in the hospital for 5 and 1/2 weeks.
Unlike the way you always imagined, your babies are now completely under the care of the hospital neonatologist (newborn specialist physician) and of the NICU nurses. You’ve now entered a strange new world, as I did three times. As I mentioned, my first set of twins were born at 30 weeks and 5 days, and stayed hospitalized for 6 weeks. My second set were born at 35 weeks, 2 days, and although my son and daughter were born more than a month later than my first set, they were still considered premature (at 4 lbs., 13 oz. and 4 lbs., 6 oz.) and were again, taken away immediately after birth to the NICU, where they stayed just over a week. My third set threatened to come early as well, and although I was the model patient who did exactly as prescribed by my doctor (and myself), my baby boys were born (believe it or not) at 30 weeks and 5 days … exactly the same gestation as my first set, but their birth weights were heavier at 3 lbs., 11 oz. and 4 lbs., 1 oz. They stayed in the hospital for 5 and 1/2 weeks.
Because I experienced NICU babies three times over the course of 12 years, I would like to share with you my advice for, not only surviving, but for the making most of your babies’ hospitalization.
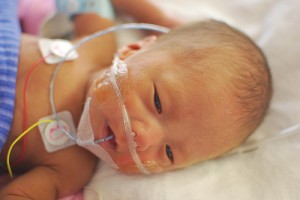 If your babies arrive early, you may be feeling …
If your babies arrive early, you may be feeling …
Completely overwhelmed: You’ve just had twins, you’re recovering from birth so you’re likely being wheeled into the NICU to meet your babies for the first time. This was NOT the way you imagined, and the entire blur of events are frightening, disappointing, painful, exhausting and bitter-sweet.
Like you are a visitor instead of your baby’s mother: Although the nurses make every effort to encourage mommy/baby bonding by allowing touch, if possible, and as close contact as medically safe, you still may feel like your baby belongs to her nurse instead of you.
That you have no control as a new mother: With all of the monitors, tubes, wires, lights flashing and alarms sounding, you feel very intimidated by this strange, mysterious and frightening place. Although you know that your baby is in the best care possible, you may feel that your role as mother has been postponed. You learn one thing for sure: your arms and hands have never been scrubbed so clean in your whole life!
Frightened and worried: Depending on the gestational age of your babies, there may or may not be medical problems related to their prematurity. As you gaze at each of your precious babies in their isolette incubators attached to tubes, monitor wires, you fear that he may never grow into the beautiful, big healthy baby you expected. Try to relax and trust that the most comprehensive medical care is being given to them, and the chances of their growing and developing normally are very, very good.
Emotional: Naturally, a brand new mother experiences the sudden drop in progesterone with the sudden rise in prolactin and oxytocin in preparation for lactation … all of which brings on the weepiness! Compound those emotions with the above listed feelings, and you may just become a (temporary) puddle of tears.
Sadness about leaving the hospital empty-armed: One of the hardest experiences for a new mother is to be discharged from the hospital and go home without your baby(ies). Those feelings of failure, loss, sadness and disappointment may kick in full-force when you return to your familiar and loving home where, when you were last there, you were still pregnant. Rest assured, however, you will have the joyful experience of walking through your front door with your babies in your arms before you know it!
My sincere and experience-backed advice
Take some deep breaths and wrap your brain around what has happened. It’s a fact that your babies have arrived, are in the best care they can possibly be, and there’s no way to turn back time. So, with that said, here are some ways to make the most of this situation.
 Find the joy in the situation: Although your birth experience was far from what you had planned or remotely expected, consider that new life has arrived, and that this indeed is a cause for celebration, albeit, a bitter sweet one. People will congratulate you … accept their congratulations graciously.
Find the joy in the situation: Although your birth experience was far from what you had planned or remotely expected, consider that new life has arrived, and that this indeed is a cause for celebration, albeit, a bitter sweet one. People will congratulate you … accept their congratulations graciously.
There are MANY ways that YOU can help your babies:
Take care of yourself: Whether you delivered vaginally or had a C-Section birth, take the time you’re home while others care for your babies to rest and heal. By the time your babies come home, you will probably be completely recovered and ready to take on the challenging and demanding role as the mom of multiples. Be sure to eat well, get enough sleep, and take good care of your own needs, because your babies are going to need you at your best.
Plan for breastfeeding by pumping your milk: You probably have made the decision to or not to breast feed your babies. Breastfeeding is the BEST nutrition for your babies, and it is very healthy for you as the next natural step in your child bearing process. Pregnancy naturally leads directly to breastfeeding. During your pregnancy, it is vital that you nourish your body the best possible way you can, both for yourself, and for your babies.
Shortly after delivery, a hospital lactation consultant visits all mothers who have indicated that they intend to breast feed their baby. In the case of your premature birth, the LC will bring a breast pump with all of the needed additional supplies into your hospital room where it will stay throughout the remainder of your stay. You will be instructed to begin pumping your first milk which is called colostrum. Colostrum is a thick yellowish substance rich in nutrition and antibodies manufactured by you specifically for your babies, and providing this perfect first food for your babies is the next, natural step in the child bearing process.
Pump, if only temporarily: If you do not plan to continue to breastfeed your babies for whatever reason, I highly recommend that mothers who deliver prematurely provide breast milk for their babies even for the first few days or weeks because the natural process of doing so connects mother with child, allowing her to feel and know that she is doing something for her babies. In fact, she’s doing the BEST THING for her babies by providing, what NICU nurses call, “liquid gold” for her premature babies. Premature breast milk is, in fact, different than full-term milk, and formulated specifically for your premature baby. From experience, pumping my breast milk for my preemies ALWAYS made me feel connected as an active contributor to the well-being and healthy growth of my babies, easing those feelings of helplessness, lack of control, guilt and disappointment caused by my early deliveries.
Be aware that you DO have a say in your babies’ care: For instance, you can specify that your babies receive only your breast milk as long as your supply is available, and to only formula feed them until you’re able to replenish the hospital’s supply when you make your next pumped milk delivery. At the same time, however, remember that your babies’ hospital stay is only temporary. If the nurses add formula or calorie boosters to your breast milk for feedings, and you don’t necessarily prefer this practice, keep in mind also that the nurses’ goal is to have your babies gain weight as soon as possible for the earliest possible discharge. Once you and your babies are home, you will make all the decisions about your babies’ care, nutrition and feeding methods.
 Once you’re home, follow a routine for pumping and storing your breast milk every three hours: Once a day you should plan to ride back to the hospital with your husband or other family member and delivery your ice-packed breast milk stored in sterile bottles provided to you by the NICU. Milk let-down reflexes and even the amount of milk you produce can be enhanced if you keep photos of your babies close by, and when you breathe in your babies’ sweet scent from their little hats or blankets that you take home from the hospital. As you had specifically labeled your pumped breast milk bottles when you were still in the hospital after delivery, you will continue to do so, so that your babies are certain to receive your milk when you return for daily visits. My husband and I referred to our trips to the hospital during our babies’ NICU stays as daily “milk-runs”!
Once you’re home, follow a routine for pumping and storing your breast milk every three hours: Once a day you should plan to ride back to the hospital with your husband or other family member and delivery your ice-packed breast milk stored in sterile bottles provided to you by the NICU. Milk let-down reflexes and even the amount of milk you produce can be enhanced if you keep photos of your babies close by, and when you breathe in your babies’ sweet scent from their little hats or blankets that you take home from the hospital. As you had specifically labeled your pumped breast milk bottles when you were still in the hospital after delivery, you will continue to do so, so that your babies are certain to receive your milk when you return for daily visits. My husband and I referred to our trips to the hospital during our babies’ NICU stays as daily “milk-runs”!
Finish preparing for your babies’ arrival: Chances are you were not fully prepared for the births of your babies when you went into premature labor and delivered them. So take this time, while your babies are hospitalized, to finish preparing the nursery, wash and fold all of your baby clothes, receiving blankets, crib sheets, etc. If you had been placed on bed rest due to your high risk pregnancy, you probably weren’t able to prepare for your babies’ arrival at all, so now you can!
Daily bonding visits: Once you feel up to it physically, plan to spend as much time with your babies as possible. Mothers are not only welcomed, but highly encouraged to spend the day with their babies. If your babies are placed together in side-by-side incubators, you may be provided a rocking chair or other comfortable chair in which to sit and breastfeed your babies for their feedings (once they reach the gestational age for gag/suck/swallow reflex coordination, at approx. 34 weeks). You can also request skin-to-skin time with your babies for further bonding. Skin-to-skin contact with their mothers increases wellness for babies. Hormones are released which calm and regulate both heart and breathing rhythm. Often, too, your babies’ nurse will encourage you to change diapers, take temperatures, prepare for feedings, and give your babies their first baths! Between feedings while your babies sleep, you can read a good book, write your birth announcements and baby gift “thank you” notes, take yourself to lunch or for a good walk around the hospital campus, or take a nap in your comfy chair before the next feeding comes around.
Bring personal items to decorate your babies’ bedside area: Bring drawings from your older children, baby clothes to have your babies dressed in, nursery items such as small stuffed animals to sit in the corner of the babies’ beds, etc., all of which allow you to feel that your babies are, in fact, YOUR babies … and that they will soon come home.
 Babies’ homecoming
Babies’ homecoming
You’ll be surprised just how quickly the time will fly before your babies are released from the hospital. Sometimes, depending upon your babies’ weights, amount of breast milk or formula that they are tolerating (keeping down), and any other medical factors, you could have as little as 12 hours release notice given by the neonatologist. Once the doctor signs the discharge orders, your baby or babies are going home! Prior to discharge, you may be required to take an Infant CPR course, which is common hospital protocol for parents. If your baby is released on the condition that he or she goes home with an apnea/bradycardia monitor to alert you of any continuing apnea episodes (that can be common with preemies, and which they outgrow with further maturation), you will be required to attend a home monitor training class. Some hospitals also require parents to “Room-in” one night with their babies in the hospital (spend a night with their baby at the hospital the night before discharge in a special room decorated like a hotel room), so that if any questions arise during the night, there are nurses available to assist.
Once you say good bye to the NICU area where you’ve spent so many weeks and take your babies home, you’ll probably wish to bring a nurse or two home with you! You may wonder why you wanted your babies to come home earlier when you’re faced with the complete, 24/7 care of your babies!
Welcome to twin parenthood!
It may have arrived at a time you hadn’t expected, but it has indeed arrived.
Congratulations … and many blessings to you and your new babies!
 2. Pregnancy Nutrition: You’ll be asked to increase your intake of iron and folic acid, along with your daily prenatal multivitamin. As with any pregnancy, you should eat foods rich in calcium, iron, and protein. It’s also very important that you drink at least two quarts of water each day to prevent dehydration, which can quickly lead to preterm labor.
2. Pregnancy Nutrition: You’ll be asked to increase your intake of iron and folic acid, along with your daily prenatal multivitamin. As with any pregnancy, you should eat foods rich in calcium, iron, and protein. It’s also very important that you drink at least two quarts of water each day to prevent dehydration, which can quickly lead to preterm labor.